Introduction
Blood sugar problems and thyroid function are two critical aspects of our overall health. They might seem unrelated at first glance, but in reality, they share a complex and interconnected relationship. Blood sugar problems, such as diabetes and insulin resistance, can significantly affect thyroid function. Understanding this relationship is essential for managing and optimizing our health. This essay explores why blood sugar problems affect thyroid function and sheds light on the intricate mechanisms behind this connection.
The Thyroid Gland and Its Functions
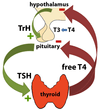
The thyroid gland, a small butterfly-shaped organ located in the neck, plays a crucial role in regulating metabolism and maintaining overall health. It produces two key hormones: thyroxine (T4) and triiodothyronine (T3). These hormones influence almost every cell in the body, affecting energy production, temperature regulation, and overall metabolic rate. To ensure proper functioning, the thyroid gland requires a delicate balance of hormones and nutrients.
Blood Sugar Problems and Their Impact
Blood sugar problems primarily refer to conditions like diabetes and insulin resistance. In diabetes, the body struggles to regulate blood glucose levels effectively. Type 1 diabetes results from an autoimmune attack on insulin-producing cells, while type 2 diabetes often develops due to lifestyle factors, including poor diet and lack of exercise. Insulin resistance, on the other hand, occurs when cells do not respond well to insulin, causing the body to produce more insulin to compensate.
The Link Between Blood Sugar and Thyroid Function
Insulin and Thyroid Hormones:
Insulin plays a pivotal role in the regulation of blood sugar levels. It facilitates the uptake of glucose into cells, allowing them to use it for energy. However, when there is excess insulin in the bloodstream, it can lead to insulin resistance. Elevated insulin levels can disrupt the delicate balance of thyroid hormones by interfering with their production and conversion.
T4 to T3 Conversion:
One essential aspect of thyroid function is the conversion of T4 to T3. T4 is the inactive form of thyroid hormone, while T3 is the active form that influences cellular metabolism. Insulin resistance and blood sugar imbalances have been linked to reduced conversion of T4 to T3. This can lead to suboptimal thyroid function and contribute to symptoms of hypothyroidism, such as fatigue, weight gain, and cold intolerance.
Inflammation and Autoimmunity:
Chronic high blood sugar levels can lead to inflammation throughout the body. This inflammation can affect the thyroid gland directly, promoting autoimmune thyroid conditions like Hashimoto’s thyroiditis. In this autoimmune disorder, the immune system attacks the thyroid, impairing its ability to produce hormones and causing hypothyroidism.
Obesity and Thyroid Function:
Obesity, often associated with blood sugar problems, can also impact thyroid function. Excess fat tissue can increase the production of inflammatory cytokines, which can disrupt thyroid hormone regulation. Furthermore, obesity can affect the distribution of thyroid hormones in the body, leading to altered metabolism.
Conclusion
In conclusion, blood sugar problems have a profound impact on thyroid function, illustrating the intricate interplay between various aspects of our health. Insulin resistance, diabetes, inflammation, and obesity can all disrupt the delicate balance of thyroid hormones, leading to suboptimal thyroid function and potential health complications. Understanding this relationship is essential for healthcare providers and individuals alike, as it emphasizes the importance of holistic health management. Managing blood sugar levels through a balanced diet, regular exercise, and proper medical care can help maintain thyroid function and overall well-being. Furthermore, addressing blood sugar issues early on can mitigate the risk of developing thyroid-related complications, underscoring the importance of proactive health management.